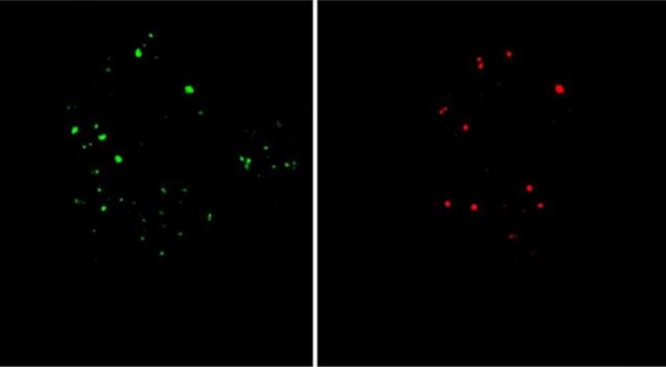
Can diet and exercise enhance gut microbiota and health in older adults? 2023
Sanjh
- 0
Intestinal bacteria and other microbes make up the gut microbiota. Microorganisms and their metabolites affect human health and immunity.
The immune system protects against germs and viruses. Infections, autoimmune, and inflammatory illnesses are more likely in elderly adults with reduced immune systems. Dysbiosis is linked to several age-related illnesses.
Age alters gut microbial composition. Diet and exercise also influence gut microbiota composition and diversity.
Scientists reviewed the literature to assess how nutrition and exercise affect gut microbiota and its activities in older persons.

Diet and aging gut microbiota
Diet regulates gut microbiota composition. Dietary variables lead gut microbiota structure to vary greatly between regions.
Non-Western immigrants to the US lose microbial diversity. Food emulsifiers alter gut microbiota makeup, causing low-grade inflammation.
The GI tract digests macro- and micronutrients, while the intestinal mucosa absorbs metabolites into the circulation. The gut microbiome controls food digestion and absorption. Diets low in nutrition can alter gut flora, causing health problems. High-fat, low-fiber diets diminish lifespan, while fiber-rich, low-calorie diets extend it.
Western diets with low fiber and excessive fat, sugar, and salt can greatly increase endotoxin-releasing bacteria, which can activate immunological responses through pathogen-associated molecular patterns. The Mediterranean diet, which is rich in vegetables, fruits, nuts, fibers, olive oil, and red wine, can boost the bacterial population that creates SCFAs and other beneficial metabolites.
Due to hunger, digestion, food sensitivity, or nutrition, older persons often vary their diet and nutrient consumption. Studies suggest that elderly persons don’t get enough vitamins and minerals for immune modulation and anti-inflammatory responses. Older folks also consume less protein, causing health issues including lean body mass loss.
Dietary changes in elderly persons cause gut microbiota dysbiosis with lower microbial diversity, butyrate-producing bacteria, and facultative anaerobic microorganisms. These alterations cause persistent, low-grade inflammation, a characteristic of many age-related illnesses.
Dietary therapies that promote gut microbiota structure and function in older persons have been studied. Some probiotics enhance helpful bacteria and decrease opportunistic microorganisms in elderly persons. In elderly individuals, prebiotic galactooligosaccharides restore gut flora and prevent inflammation.
According to the researchers, additional research is needed to determine how food affects gut microbial composition and function in older persons. Well-controlled studies are needed to uncover gut microbiota-modulating dietary treatments that enhance aging populations’ health.
Exercise and aging gut microbiota
Regular exercise reduces the risk of cardiovascular and metabolic illnesses and all-cause mortality, improving cardiorespiratory fitness and general health. Inflammation and immune senescence cause high-mortality illnesses in older persons. Regular exercise reduces chronic, low-grade inflammation, improves immunological function, and increases autophagy (a cellular mechanism to destroy and eliminate cellular trash), lowering the risk of many illnesses.
Exercise alters gut microbiota composition and diversity. These studies did not control for food, age, or exercise training program, therefore they could not assess how exercise affects gut flora.
One well-controlled animal investigation found that six weeks of voluntary wheel running lowers gut microbiota richness in young mice compared to treadmill running or inactive circumstances. However, forced treadmill running enriches GI tract-pathogenic endotoxin-producing bacteria in mice.
The study indicated that exercise may help or harm gut microbiota depending on stimulus.
Exercise improves gut microbiota function in rugby players. Gut microbiota composition and diversity are strongly connected with athletes’ cardiorespiratory fitness. Cardiorespiratory fitness is also linked to SCFA production, bacterial chemotaxis, and motility genes.
Depending on BMI, six weeks of endurance exercise changes gut microbiota and SCFA levels in young adults. Eight weeks of endurance and resistance training in healthy people did not modify gut microbiota composition, function, or microbial diversity.
These investigations suggest further longitudinal research to determine how exercise affects gut microbiota and its effects, especially in older people.